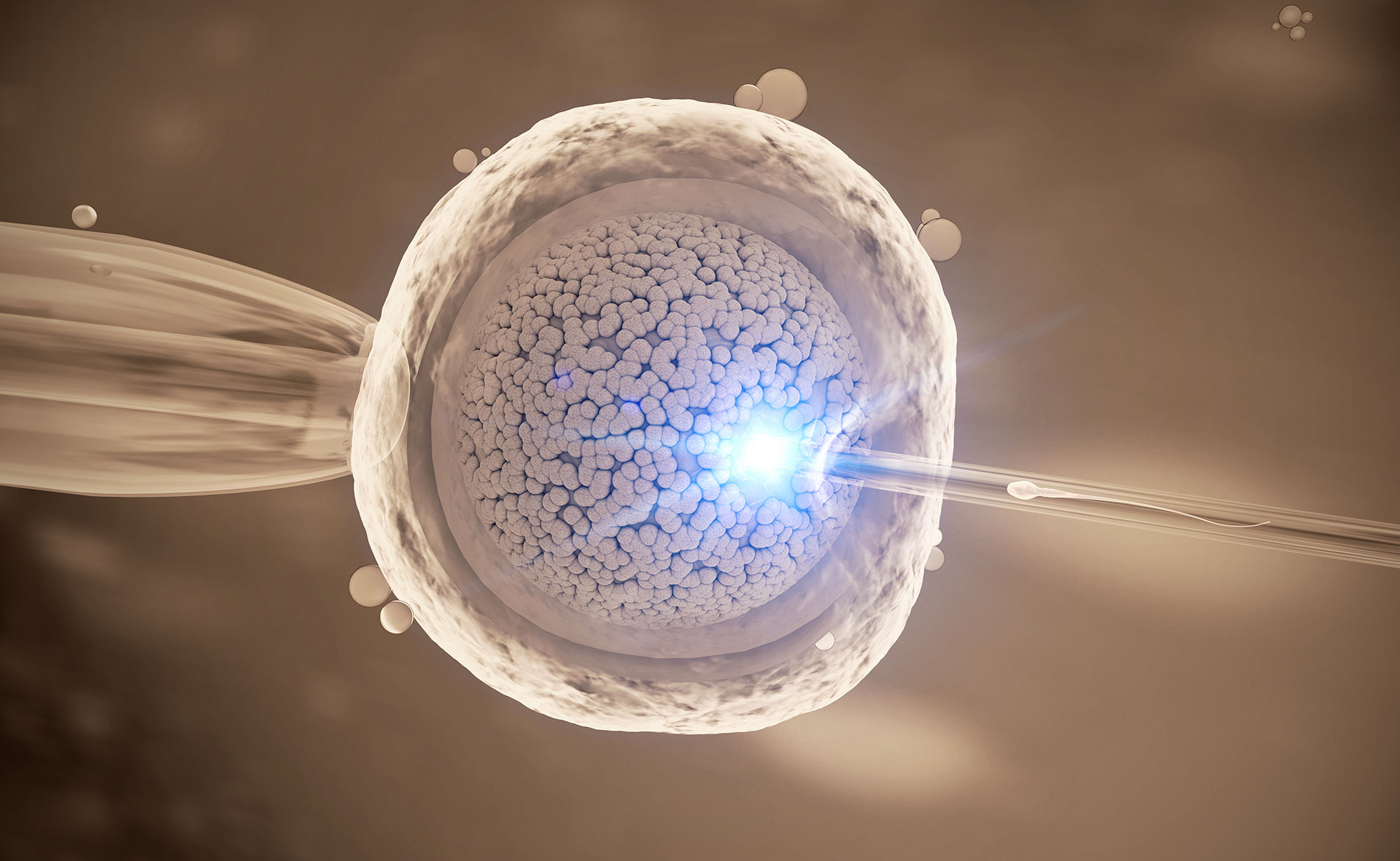
Τι είναι;
Η εξωσωματική γονιμοποίηση (IVF) ήταν η πρώτη τεχνική υποβοηθούμενης αναπαραγωγής (ART) που εφαρμόστηκε και εξακολουθεί να είναι η πλέον ευρέως χρησιμοποιούμενη.
Ποια είναι η διαδικασία;
Στα πλαίσια ενός κύκλου IVF, τα ωάρια (τα οποία συνήθως προκύπτουν μετά από την ελεγχόμενη διέγερση των ωοθηκών με την βοήθεια ορμονικών σκευασμάτων) και τα σπερματοζωάρια συλλέγονται και τοποθετούνται μαζί σε ένα τρυβλίο ώστε να πραγματοποιηθεί η γονιμοποίηση. Αν τα ωάρια γονιμοποιηθούν επιτυχώς στο εργαστήριο, μεταφέρονται στη μήτρα της γυναίκας. Ιδανικά, ένα από τα γονιμοποιημένα ωάρια θα εμφυτευθεί στη μήτρα και θα αναπτυχθεί, όπως συμβαίνει φυσιολογικά.
Στάδια Εξωσωματικής Γονιμοποίησης IVF
Η εξωσωματική γονιμοποίηση (IVF) διακρίνεται σε τέσσερα στάδια:
Διέγερση ωοθηκών – Παρακολούθηση & πρόκληση ωοθυλακιορρηξίας
Οι πιθανότητες επίτευξης κύησης αυξάνονται με την παρουσία μεγάλου αριθμού ώριμων ωαρίων, διαθέσιμων προς γονιμοποίηση. Δεδομένου ότι φυσιολογικά, το γυναικείο σώμα αναπτύσσει και ελευθερώνει μόνο ένα ώριμο ωάριο κάθε μήνα, η ανάπτυξη περισσότερων ωοθυλακίων είναι δυνατή μόνο μετά από τη χρήση εξωγενώς χορηγούμενων ορμονικών σκευασμάτων που προκαλούν ελεγχόμενη υπερδιέγερση των ωοθηκών και άρα ανάπτυξη πολλών ωοθυλακίων. Τα ωοθυλάκια είναι σάκοι γεμάτοι με υγρό μέσα στους οποίους αναπτύσσονται και ωριμάζουν τα ωάρια. Για την ρήξη του ωοθυλακίου (ωοθυλακιορρηξία,) την τελική ωρίμανση και ελευθέρωση των ωαρίων χρησιμοποιούνται επίσης ορμονικά σκευάσματα και πιο συγκεκριμένα, σκεύασμα ανθρώπινης χοριακής γοναδοτροπίνης.
Η γυναίκα υποβάλλεται σε υπερηχογραφικό έλεγχο σε τακτά χρονικά διαστήματα προκειμένου να εξεταστεί ο αριθμός και το μέγεθος των ωοθυλακίων που αναπτύσσονται. Δεδομένου ότι τα αναπτυσσόμενα ωοθυλάκια εκκρίνουν αυξανόμενες ποσότητες οιστρογόνων, απαιτείται επίσης συχνός βιοχημικός έλεγχος για την παρακολούθηση των ορμονικών επιπέδων με στόχο τον προσδιορισμό του ιδανικού χρόνου για τη χορήγηση του σκευάσματος hCG ώστε να επιτευχθεί η τελική ωρίμανση των ωαρίων πριν την ωοληψία.
Λήψη ωαρίων
Από τη στιγμή που η διέγερση των ωοθηκών έχει ολοκληρωθεί και τα ωοθυλάκια ωριμάσουν, θα ακολουθήσει η συλλογή των ωαρίων που έχουν αναπτυχθεί. Η διαδικασία αυτή, η οποία είναι γνωστή ως ωοληψία είναι σύντομη και πραγματοποιείται υπό ελαφρά γενική αναισθησία. Τα ώριμα ωοθυλάκια εντοπίζονται υπερηχογραφικά και στη συνέχεια εισάγεται στον κόλπο μία βελόνα για τη λήψη του υγρού από το ώριμο ωοθυλάκιο με ήπια αναρρόφηση. Το υγρό εξετάζεται άμεσα με τη βοήθεια μικροσκοπίου ώστε να επιβεβαιωθεί η λήψη ωαρίου. Η εν λόγω διαδικασία επαναλαμβάνεται για κάθε ένα από τα ώριμα ωοθυλάκια και στις δύο ωοθήκες. Όσα ωάρια λαμβάνονται από το ωοθυλακικό υγρό τοποθετούνται σε επωαστικό θάλαμο.
Για την καλύτερη προετοιμασία του τοιχώματος της μήτρας για την φιλοξενία του γονιμοποιημένου ωαρίου συχνά προτείνεται η εξωγενής χορήγηση προγεστερόνης, οιστρογόνου και παιδικής ασπιρίνης, μετά την ωοληψία.
Γονιμοποίηση ωαρίου
Δύο ώρες περίπου πριν τη λήψη των ωαρίων, λαμβάνεται δείγμα σπέρματος από τον σύντροφο της γυναίκας ή από τον δότη. Το δείγμα αυτό υποβάλλεται σε ειδική επεξεργασία ώστε να ενεργοποιηθεί. Στη συνέχεια, τα σπερματοζωάρια τοποθετούνται μαζί με τα ωάρια σε έναν επωαστικό θάλαμο που έχει ρυθμιστεί ώστε να έχει κατάλληλες συνθήκες θερμοκρασίας, πίεσης κ.λπ. Την επόμενη μέρα, τα ωάρια εξετάζονται μικροσκοπικά, ώστε να προσδιοριστεί αν έχει συντελεσθεί γονιμοποίηση. Στην συνέχεια, τα γονιμοποιημένα ωάρια που θα προκύψουν θα παραμείνουν για κάποιο διάστημα στο εργαστήριο ώσπου να κριθούν έτοιμα προς μεταφορά στη μήτρα μέσα σε περίπου 72 ώρες.
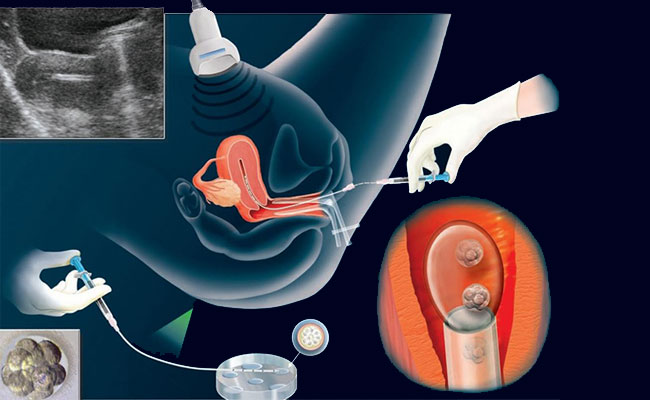
Εμβρυομεταφορά
Η εμβρυομεταφορά (μεταφορά των εμβρύων που έχουν αναπτυχθεί στο εργαστήριο) δεν είναι περίπλοκη διαδικασία και μπορεί να πραγματοποιηθεί χωρίς αναισθησία. Τα έμβρυα τοποθετούνται σε έναν σωλήνα- καθετήρα και μεταφέρονται στη μήτρα από 2 έως 6 ημέρες μετά την ωοληψία. Όταν η μεταφορά των εμβρύων γίνεται την 5η ή 6η μέρα από την ωοληψία τα έμβρυα έχουν φτάσει στο στάδιο των βλαστοκύστεων (12- 150 κύτταρα).
Ο αριθμός των μεταφερόμενων εμβρύων εξαρτάται από:
- την ηλικία της γυναίκας
- το αίτιο υπογονιμότητας
- το πιθανό προηγούμενο ιστορικό κυήσεων
- άλλους παράγοντες
Αν υπάρχουν επιπλέον έμβρυα που είναι εξαιρετικής ποιότητας, ενδέχεται να πληρούν τις προϋποθέσεις συντήρησης υπό συνθήκες ψύξης (κρυοσυντήρηση) για μελλοντική χρήση.
Άλλες τεχνικές εξωσωματικής γονιμοποίησης
Στο ιατρείο εξωσωματικής γονιμοποίησης που διευθύνουμε, επί σειρά ετών προσφέρουμε με συνέπεια και υπευθυνότητα εξειδικευμένες υπηρεσίες που σχετίζονται με:
- Ενδοκυτταροπλασματική έγχυση σπερματοζωαρίου (ICSI)
- Εξωσωματική ωρίμανση ωαρίων (In Vitro Maturation – IVM)
- Δωρεά ωαρίων
- Προεμφυτευτική διάγνωση
Όλα όσα θέλετε να μάθετε για την Εξωσωματική Γονιμοποίηση IVF
Ποιο είναι το ποσοστό επιτυχίας της εξωσωματικής γονιμοποίησης;
Για την αντιμετώπιση του προβλήματος της υπογονιμότητας η σύγχρονη ιατρική επιστήμη έχει αναπτύξει τα τελευταία 30 χρόνια εξελιγμένες θεραπευτικές μεθόδους υποβοήθησης της αναπαραγωγής.
Η αντιμετώπιση της υπογονιμότητας με τις θεραπείες αυτές οδηγεί σε ποσοστά κύησης που κυμαίνονται στο 35-40% για κάθε προσπάθεια, ανάλογα βέβαια με το είδος του προβλήματος, την ηλικία της ασθενούς κλπ. . Μάλιστα, αθροιστικά το ποσοστό αυτό αυξάνεται σημαντικά και ανέρχεται στο 70- 80% μετά από 3 κύκλους θεραπείας γεγονός που συνεπάγεται ότι το μεγαλύτερο ποσοστό των ζευγαριών που θα καταφύγουν σε ένα ειδικό κέντρο αποκατάστασης της γονιμότητας θα επιστρέψει τελικά στο σπίτι του με ένα παιδί.
Αν, δε, λάβουμε υπόψη μας ότι η μέση πιθανότητα σύλληψης ενός γόνιμου ζευγαριού είναι της τάξης του 15-20% για κάθε μήνα της ζωής του, γίνεται κατανοητό ότι οι σύγχρονες τεχνικές υποβοήθησης της αναπαραγωγής προσφέρουν πολύ αξιόλογα ποσοστά επιτυχίας που βρίσκονται πολύ κοντά σε αυτά που προσφέρει η φύση σε ζευγάρια χωρίς κανένα πρόβλημα τεκνοποίησης.
Πόσες φορές μια γυναίκα μπορεί να υποβληθεί σε θεραπεία εξωσωματικής γονιμοποίησης;
Ο αριθμός των κύκλων θεραπείας στους οποίους μπορεί να υποβληθεί μια γυναίκα δεν είναι καθορισμένος. Είναι βέβαιο ότι στη χώρα μας υπάρχουν υψηλού επιπέδου μαιευτήρες- γυναικολόγοι και οργανωμένα κέντρα θεραπείας υπογονιμότητας που προσφέρουν άψογες ιατρικές υπηρεσίες σε αυτό το επίπεδο.
Εφόσον υπάρχουν σωστές ενδείξεις (π.χ. ωοθήκες που ανταποκρίνονται στην θεραπεία διέγερσης, καλής ποιότητας ενδομήτριο κλπ.) το ποσοστό επιτυχίας, ιδιαίτερα με τη χρήση των νεώτερων τεχνικών και βιοτεχνολογικών φαρμάκων που παρουσιάζουν αυξημένη βιοδραστικότητα συγκριτικά με τα συμβατικά φάρμακα από ούρα, ανέρχεται αθροιστικά περίπου στο 65-70% μετά από 3 κύκλους θεραπείας.
Καθώς έχουν περάσει 40 χρόνια από την γέννηση του πρώτου IVF μωρού ποιες είναι οι πιο σημαντικές εξελίξεις και που οδεύει η επιστημονική αντιμετώπιση του προβλήματος;
Εξ ορισμού, η αντιμετώπιση της υπογονιμότητας είναι πολυπαραγοντική. Ετσι, σημαντικά βήματα εξέλιξης έχουμε σε όλους τους επιμέρους τομείς, όπως;
- στη διαγνωστική προσέγγιση του ζευγαριού, όπου η εφαρμογή των ενδοσκοπικών τεχνικών έχει γενικευτεί και η διερεύνηση ανοσολογικών προβλημάτων είναι επαρκέστερη.
- σε τεχνικά ζητήματα π.χ. βελτίωση των καλλιεργητικών υλικών που απαιτούνται στο εργαστήριο καθώς και το quality control του εμβρυολογικού εργαστηρίου
- στην υιοθέτηση νέων πρακτικών μεθόδων όπως η προεμφυτευτική διάγνωση, οι βλαστοκύστεις, η μεταμόσχευση κυτταροπλάσματος, in vitro maturation κλπ.
- στην φαρμακευτική αγωγή και τα σκευάσματα που χρησιμοποιούνται, όπου έχουν πραγματικά γίνει άλματα προόδου και εξέλιξης
Καλύπτουν τα ασφαλιστικά ταμεία το κόστος της θεραπείας IVF;
Τα τελευταία χρόνια η πολιτεία έχει δει θετικά το πρόβλημα της υπογονιμότητας με αποτέλεσμα να βελτιώσει την πρόσβαση των υπογόνιμων ζευγαριών στις σύγχρονες ιατρικές Τεχνικές Υποβοήθησης της Αναπαραγωγής. Έτσι πλέον τα περισσότερα ασφαλιστικά ταμεία καλύπτουν ικανοποιητικά το κόστος της φαρμακευτικής αγωγής για περιορισμένους κύκλους θεραπείας. Για περισσότερες πληροφορίες απευθυνθείτε στο ασφαλιστικό σας ταμείο ή στον ασφαλιστικό σας σύμβουλο.
Θέλετε να μάθετε περισσότερα για την Εξωσωματική Γονιμοποίηση IVF; Κλείστε ραντεβού και ο κ. Γιατράς θα λύσει όλες σας τις απορίες.